Facial disfigurements can have drastic effects on any individual. With already a multitude of stresses at play, diagnosing a problem in such cases is quite challenging. The orthognathic surgeon can be faced with both smooth and difficult encounters when they first see their patients.
By Dr Saqba Alam
LOOKING AT AN ASYMMETRIC PATIENT
The dentofacial deformities affect up to 30% of individuals worldwide, having varying degrees of both functional and esthetic deficits. The assessment requires a multidisciplinary team for successful outcomes. To have a healthy relationship with such patients, it is mandatory to approach these patients in a gentle, calming manner maintaining good eye contact throughout that not only will build a good rapport but will also aim to extract all necessary information from the patient to reach an accurate diagnosis; which is the fundamental goal in good treatment planning. Good consultation skill includes self-evaluation, questioning skills, listening skills, giving information, non-verbal communication skills. Simultaneous 3D thinking is crucial when listening to such patients as the dentofacial deformities are interrelated with adjacent anatomic structures and require careful evaluation of both function and asymmetry.
HISTORY AND EXAMINATION
With a professional demeanour tailored to the ongoing clinical scenario, the physician should lead the way to a thoughtful discussion in obtaining precise historical details from the patient. A set of questionnaires for an orthognathic patient is readily available online but can be customized for different cases accordingly. Breathing evaluation, snoring and sleep patterns, type of food intake notice any enlarged turbinates or adenoids, significant TMJ history of clicks and popping sounds, symptoms of mouth breathing, symptoms of sinusitis, past medical, dental and surgical history. A history of any hereditary defects, syndromes, and clefts must be mentioned in the patients' orthognathic records. At the end of the consultation, the clinician should ask a general question if the patient’s expectations regarding the consult were fulfilled and allow the patient to respond to the question.
The orthognathic patient can have variable degrees of compromise in their head and neck functions, including chewing, speech, swallowing, breathing, TMJ pains, Obstructive sleep apneas, posture disturbances, malocclusion and lip closure. The attending clinician should also try to assess the patients’ expectations and compliance with the treatment. Obtaining complete biodata and age is essential to determine the role of myofascial appliances in growing individuals. It is crucial to know the patient's peak pubertal age and skeletal maturation age before proceeding towards surgery.
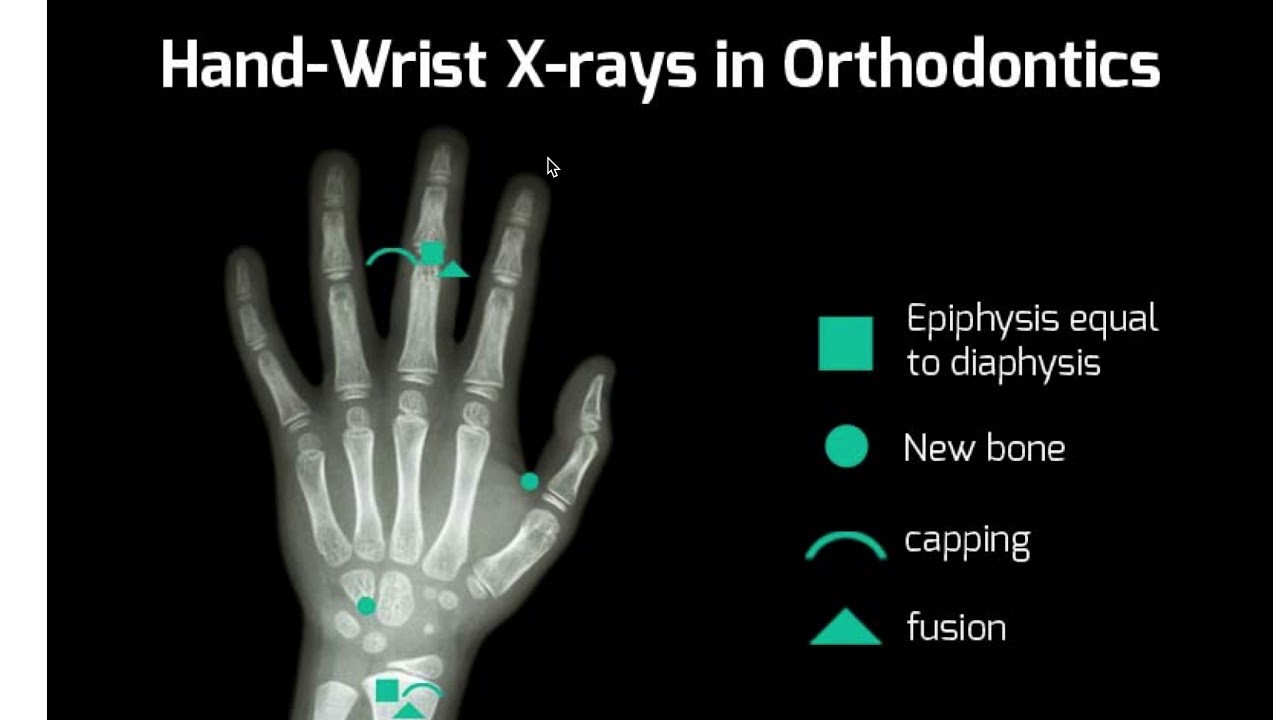
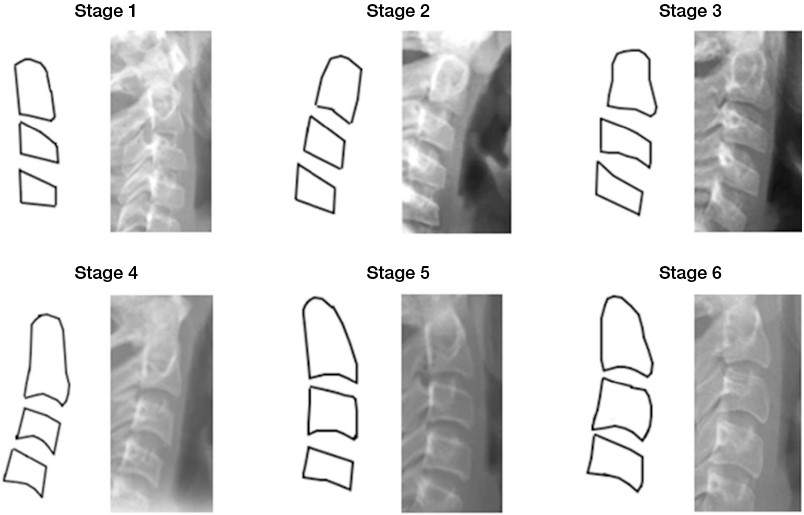
Some of the good indicators are the appearance of sesamoid bone and fusion of epiphyseal and diaphyseal plates, and the fusion of the radius on the hand wrist x rays. Another great maturation indicator is the inferior border notching and increases in C2 C3and C4 vertebrae's height on cervical x-ray films. Reproducible lateral cephalometric x rays can be done for the same purpose.

The clinical examination begins with the patients’ head in the Natural Head Position (NHP), lips relaxed and the Frankfort Horizontal parallel to the floor.Frontal and lateral views of the patient holds importance.On general inspection an estimate of patients’ profile, head shape and asymmetric proportions can be ruled out. After this crucial step, various angles and analysis can be performed on Cephalometric tracings to add to the clinical diagnosis.
A systematic bottom-up or top-down approach is helpful to examine in an organized manner without missing any key features. Extraoral examination of hard and soft tissues should be performed first after dividing the face into three sections(hairline to glabella, glabella to sub nasale and subnasale to most prominent point on chin). Facial growth comparison on both ipsilateral and contralateral sides is essential for some syndromic conditions like Parry Romberg or facial atrophic conditions. Beginning from Top, the facial and dental midlines, hair shape, forehead height, pupillary and globe levels, ear symmetry, nasal symmetry and deviation, zygoma fullness and bizomatic width, alar base width, lip length, lip fullness, gingival and incisal show, chin projection, tracheal deviation, neck symmetry and a rough estimate of the skeletal discrepancy (excess or deficiency )on lateral view is vital.
IMAGING:
Clinical photographs are helpful for documentation and photometric analysis. Radiographic interpretation using only Panorex and Cephalometric X rays are not considered complete at the present times in orthognathic surgery. Nowadays, 3D imaging is leading to broader possibilities. Digital planning enhances diagnostic accuracy.
VIRTUAL SURGICAL PLANNING USING 3D CT:
The 2D imaging though informative but fails to interpret the third dimension,i-e depth of anatomic structures etc. At present, intraoral scanners have made it possible to have an immediate, accurate digital model of the dental arches.
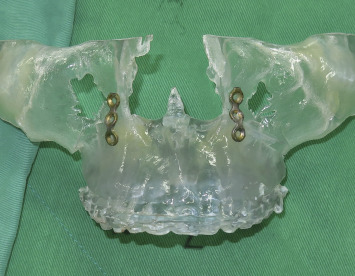
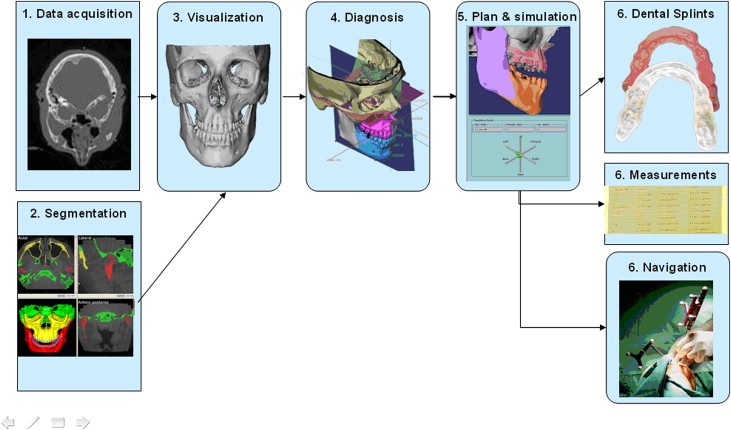
The integration of 3D data from different anatomical structures (skeleton, dentition and facial soft tissues) allows to obtain a 3D virtual simulation of a patient, as well as to simulate the treatment outcome into the patients’ faces, thus leading to better communication with colleagues, technicians and patients (DICOM)Digital Imaging and Communication in Medicine.
The Computer-Aided Surgical Simulation (CASS) planning method generates 3D computer composite skull models and orients them to the neutral head posture. These models undergo virtual surgeries. Skeletal harmony achieved with CASS is significantly better than that achieved with traditional methods.
PRESURGICAL PLANNING AND DECOMPENSATION:
Presurgical Orthodontics aims to achieve arch coordination, levels and align the teeth. Compensations are natures’ attempt at camouflaging a jaw deformity.
Arch is normalized when teeth are orderly arranged, and there is no tipping, displacement or rotation; dental compensations have been removed, and the Curve of Spee is made flat or minimal. The arches should correspond to each other, and all interdental spaces are closed with orthodontics.
OSTEOTOMY:
During the past three decades, significant advances in surgical osteotomy techniques and instrumentation, such as the use of Piezo aids have been developed and carried out in orthognathic surgery. However, the primary surgical principles have more or less remained unchanged. After recent advances in Computer Assisted surgery, it has been possible to predict the treatment results.
Detailed surgical planning is essential for a successful outcome. The treatment involves:
• An accurate treatment plan.
• The correct type of instruments for a specific procedure.
• Proper splints.
• Protocol for each osteotomy design and strict adherence to the basic anatomic knowledge and surgical guidelines.
Various Osteotomy designs have been described both for the maxilla and mandible. Le Fort I, II, III osteotomies, segmental osteotomies of the maxilla, bilateral sagittal split osteotomy (BSSO), bilateral vertical osteotomy (BVO) genioplasty, segmental osteotomy of the mandible.
At the termination of jaw osteotomies, additional polishing procedures like genioplasty, pyriformplasty, and septoplasty can help add stability reduce chances of relapse.
POST SURGICAL ORTHODONTICS:
The post-surgical phase of any orthognathic surgery typically begins 4-8 weeks after the surgical procedure and typically lasts 2-6 months. This short phase is necessary to detail the final occlusion. The goal is to maintain the teeth in occlusion and provide stability and correct any possible skeletal relapse. Post-surgical retainers are given.
POST OP FINISHING PROCEDURES:
These can be described as final strokes of the brush and are targeted upon creating that last beautiful look of the patient. Finishing procedures most often call for multidisciplinary, or even transdisciplinary, collaboration. The good alliance between the surgeon and orthodontist is crucial. These procedures may include the use of Botox and Fillers, dental and prosthetic implants, fat grafting, liposuction, blepharoplasty and cosmetic lifts.
The author is an FCPS finalist for Oral Maxillofacial Surgery. She has completed her residency at Abbasi Shaheed Hospital and previously worked at Agha Khan University Hospital, Liaquat National Hospital, and Manchester UK. She has worked as a Registrar in the Department of Oral Maxillofacial Surgery at Altamash Medical Hospital Clifton. She is currently working at an aesthetic clinic and can be reached at drsaqbaalam@gmail.com

Dr Muattar Hanif
The author is Editor at Dental News Pakistan and can be reached at newsdesk@medicalnewsgroup.com.pk

